 In the absence of such events, one should search for a remediable cause of the concerning FHR tracing. 12.10) could have occurred secondary to umbilical cord prolapse, placental abruption, or uterine rupture. For example, an acute change in the FHR pattern with prolonged deceleration ( Fig. The evaluation of a category II or III pattern begins with a search for an underlying etiology that would itself require immediate delivery. Martin MBBS, FRACP, in Fanaroff and Martin's Neonatal-Perinatal Medicine, 2020 Management of Non–Category I FHR Patterns During Labor Fetal acidosis is more likely if baseline variability is absent. For fetal heart rates between 160 and 180 beats/min, the presence or absence of baseline variability is an important indicator of fetal acid-base status. Fetal heart rates above 200 beats/min, and certainly above 220 beats/min, should increase the index of suspicion of fetal tachyarrhythmia and lead to further fetal cardiac evaluation with a targeted fetal echocardiogram. Other causes include chronic hypoxemia, maternal hyperthyroidism, and fetal tachyarrhythmia. The most common etiology of fetal tachycardia is maternal-fetal fever secondary to maternal-fetal infection such as chorioamnionitis. Vagal activity has a greater influence on fetal heart rate at baseline as gestation advances thus baseline fetal heart rate will decrease from an average of 155 beats/min at 20 weeks to 145 beats/min at 30 weeks. The fetal heart rate baseline evaluation must also take gestational age into account, as with fetal heart rate reactivity. Druzin, in Obstetrics: Normal and Problem Pregnancies (Seventh Edition), 2017 Tachycardia 79 Prolonged decelerations (60 seconds) are associated with fetal acidemia and are extremely ominous, particularly with the absence of variability. 78 In general, minimal-to-undetectable FHR variability in the presence of variable or late decelerations is associated with fetal acidosis. 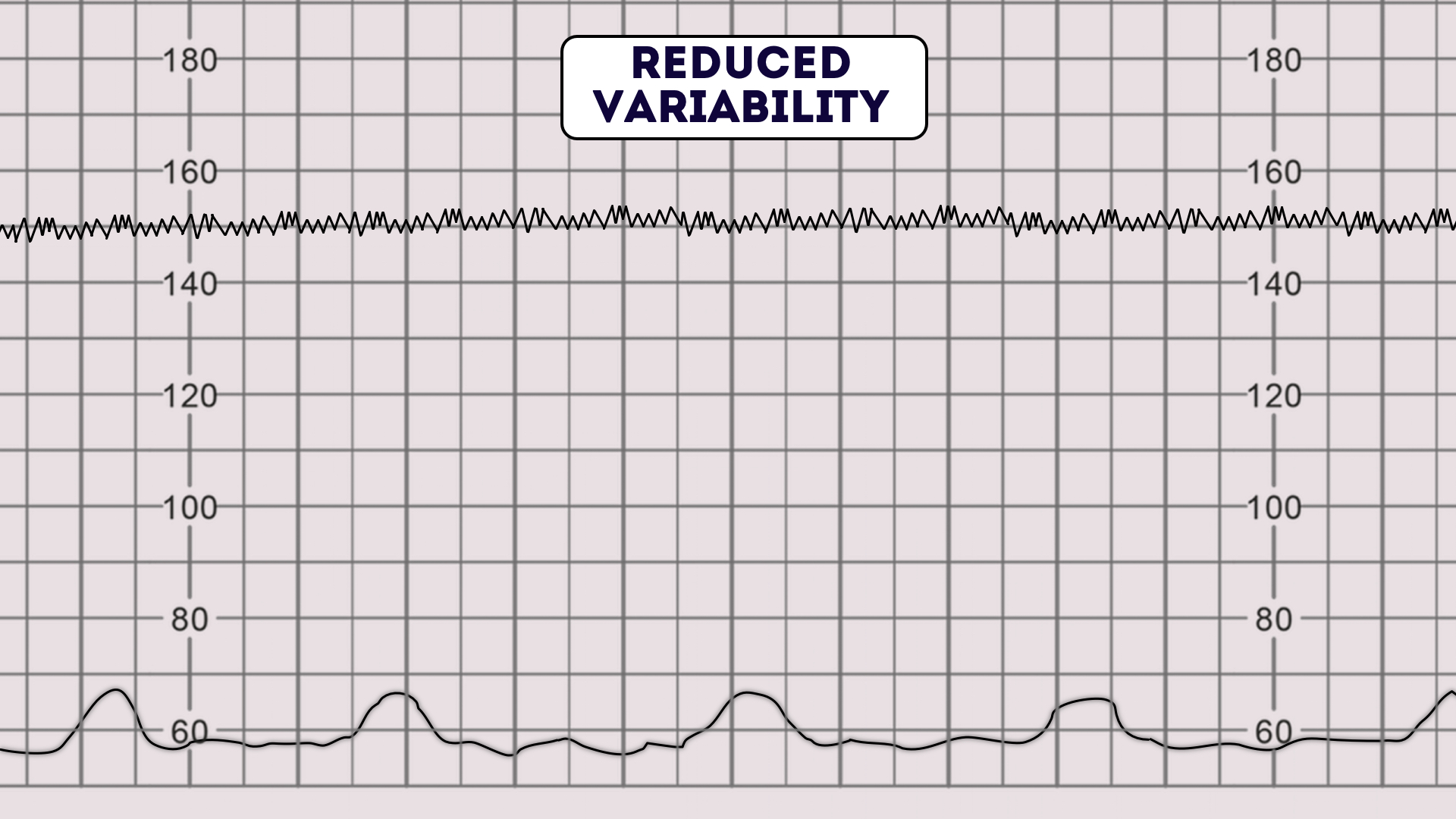
A sinusoidal FHR pattern is associated with fetal anemia and is considered ominous. Variable decelerations are associated with umbilical cord compression. On the other hand, early decelerations are considered benign and tend to mirror the uterine contraction and are believed to be in response to vagal stimuli, which are often the result of fetal head compression. 77 Therefore late decelerations are considered worrisome. A second type of late deceleration is from myocardial depression in the presence of increasing hypoxia. The resulting sympathetic outflow elevates the fetal blood pressure and activates the fetal baroreceptors and an associated slowing in the FHR. Late decelerations are a result of uteroplacental insufficiency causing relative fetal brain hypoxia during a contraction. 62.3 details FHR tracing deceleration characteristics. Accelerations are abrupt changes in the FHR above baseline and are defined by gestational age of the fetus.įig. Normal FHR variability predicts early neonatal health and a fetal central nervous system that is normally interacting with the fetal heart. FHR variability are fluctuations in the baseline FHR that are irregular in frequency and amplitude. A normal baseline FHR ranges from 110 to 160 bpm. Box 62.1 defines FHR baseline, variability, and accelerations. It should be interpreted over a time course in relation to the clinical context and other known maternal and fetal comorbidities, because multiple factors other than fetal acidosis can influence the FHR tracing. The FHR tracing is used as a nonspecific reflection of fetal acidosis. 76 These changes in the FHR produce specific patterns and characteristics that provide an evaluation of the fetal state. 76 It also shows changes as a result of various fetal brain metabolic changes that occur with asphyxia. The FHR pattern changes in response to fetal asphyxia from activation of peripheral and central chemoreceptors and baroreceptors. Of note, a fetal scalp electrode can be placed only if the cervix is minimally dilated and the membranes are ruptured. For internal monitoring, a peak or threshold voltage of the fetal R wave from the scalp electrode is used to measure FHR. 
Gropper MD, PhD, in Miller's Anesthesia, 2020 Fetal Heart Rate TracingįHR monitoring is most commonly accomplished with a surface Doppler ultrasound transducer (external monitoring), but it may be necessary to apply a fetal scalp electrode to obtain accurate continuous FHR monitoring (internal monitoring). 
0 Comments
Leave a Reply. |
Details
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
